A guide to getting “the good” from generative AI while understanding and dodging “the bad.”…
From Plate to Practice: Addressing the Barriers to the Mediterranean Diet in Older Adults
The Mediterranean diet is often hailed as a gold standard for health, but its true impact depends on one critical factor: long-term adherence. Without addressing the barriers that prevent lasting change, even the best dietary recommendations fall short.
by Roxanne Bennett, MSc; Isabelle Lussier, PhD; Juliette Guillemont, MSc; Sylvie Belleville, PhD ; Guylaine Ferland, PhD
The Mediterranean Diet and Its Challenges for Long-Term Adherence
What we eat is increasingly recognized as an important factor in how we age and in our risk for chronic diseases. Among the dietary patterns most widely studied, the Mediterranean diet (MedDi) stands out for its consistent links to long-term health outcomes, including healthy aging and a reduced risk of cognitive decline. First described in the traditional eating habits of countries such as Greece before the 1960s, the MedDi is now understood more broadly as an eating pattern that emphasizes extra-virgin olive oil as a main source of fat, along with a high intake of vegetables, fruits, whole grains, nuts, and legumes. It also includes moderate amounts of fish and dairy and limits sweets, eggs, meat and meat products. Over the past few decades, the MedDi has gained international recognition for its wide-ranging health benefits. For example, both the Alzheimer Society of Canada and the Alzheimer’s Association in the United States include it in their recommendations for maintaining brain health and reducing the risk of cognitive decline.
The Roadblocks to Adoption: Why the Mediterranean Diet may be Difficult for Older Adults
Making long-term changes to diet is notoriously difficult, and dietary recommendations only work if people can successfully follow and maintain them. Middle-aged and older adults may face several challenges, including the difficulty of changing long-standing eating patterns, especially when the recommended diet has roots in a different cultural context. Yet, research addressing these barriers in middle-aged or older adults and the MedDi is limited and the findings remain fragmented.
The Luci Project: Supporting Healthy Aging Through Lifestyle Changes
The Luci project, launched in Canada in 2020, was designed to promote healthy aging. It is a fully remote, personalized web-based behavioral intervention designed to help individuals adopt healthy lifestyle habits, with optional guidance from trained coaches. Luci was created after philanthropist André Chagnon set out to develop a technology-driven solution to help prevent cognitive decline, after losing his wife Lucie to Alzheimer’s in 2014. The Luci program focuses on three key domains: a Mediterranean-style diet, physical activity, and cognitive engagement. The program’s educational content, coaching methods, and platform tools were developed to provide an evidenced-based approach to changing lifestyle habits.
This work reflects a “From Plate to Practice” approach, integrating dietary guidance and scientific evidence with real-world, practical behavior strategies to support meaningful change. To guide the dietary component of the program, we reviewed past studies on the barriers to adopting the MedDi in middle-aged and older adults residing in non-Mediterranean regions, such as North America, Northern Europe, and Australia. We then drew these results together, looking for similarities and shared themes across studies, to provide a broader, more evidence-based foundation for program development.
How Can the Behavior Change Wheel Help Us Understand Dietary Barriers?
To combine results from many studies, it is important to use an organized method to compare their findings. We used the Behavior Change Wheel (BCW) because it not only helps organize findings but also guides the selection of effective behavior change strategies. The BCW is a widely used, well-validated behavior change framework developed to assist in designing successful interventions.
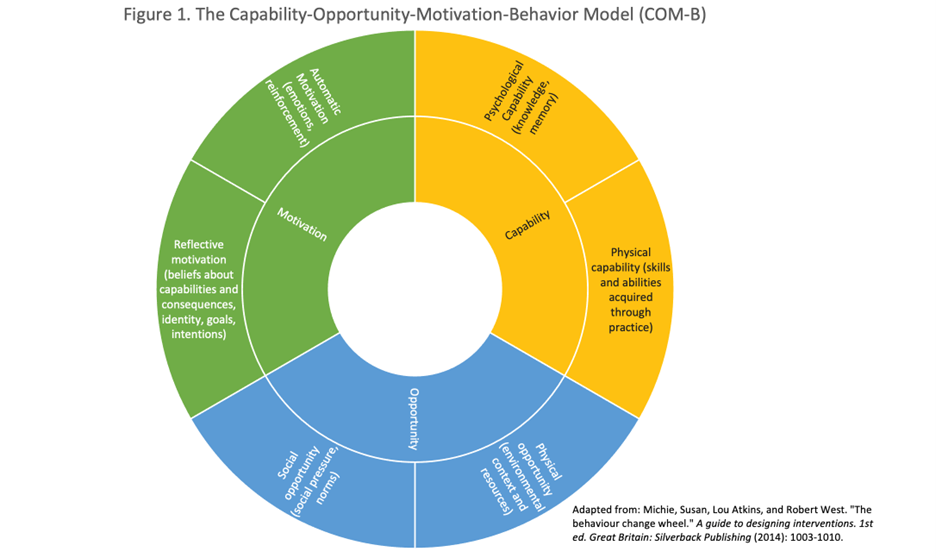
Adapted from The behavior change wheel by Michie et al. (2011), CC BY 4.0
At the heart of BCW is the COM-B model, which stands for Capability-Opportunity-Motivation (COM-B). Simply put, it explains that for any behaviour to happen, a person needs to have the ability to do it (Capability), the chance to do it (Opportunity), and the desire to do it (Motivation). The COM-B helps identify what needs to change for a behavior to occur. By pinpointing the internal (e.g., psychological) and external (e.g., environmental) factors that influence behavior, the COM-B model helps guide the choice of suitablestrategies to support behavior change (sometimes referred to as “intervention functions”).
Research Findings: Key Barriers to the Mediterranean Diet in Older Adults
Our initial suspicion regarding the limited research on this topic was confirmed when out of the 252 studies identified in our search, only four met our inclusion criteria.All were qualitative studies, with three conducted in the UK and one in Australia. Qualitative research focuses on exploring people’s experiences, opinions, and perspectives, providing insights that numbers alone cannot capture.
Summary of the Included Studies
| Year | Country | Participants | |
| Study 1 | 2015 | United Kingdom | 11 adults between the ages of 50-65 shared their perspectives following an 8-week MedDi intervention. |
| Study 2 | 2018 | United Kingdom | 67 adults with multiple risk factors for heart disease (but no diagnosis) participated in focus groups on their perceptions of the MedDi. |
| Study 3 | 2019 | United Kingdom | 19 adults with non-alcoholic fatty liver disease (NAFLD) reflected on the challenges they experienced during a 12-week MedDi intervention. |
| Study 4 | 2020 | Australia | 17 adults aged 55 and over discussed their experience after a 2-week MedDi trial. |
Using established research methods for analyzing qualitative research, we carefully reviewed and grouped findings from different studies and were able to identify the following descriptive themes, classified into their corresponding COM-B model categories.
Capability
Capability refers to an individual’s ability to perform a specific behavior, which may be physical (including strength and coordination) or psychological (knowledge and practical skills).
- Psychological capability: Low nutrition competencies were reported in all studies:
- Many felt they didn’t know enough about the MedDi or what it includes, some had misunderstandings, such as worrying it might cause weight gain;
- Many struggled to find reliable or trustworthy nutrition information;
- In two studies, participants felt they didn’t have enough cooking or food skills to prepare MedDi foods or meals;
- Another study found that some people struggled to read food labels and identify healthier options.
- Physical capability: In one study, some participants reported that physical limitations (like reduced mobility or difficulty with daily tasks) made it harder to adopt the MedDi.
Opportunity
Opportunity encompasses external factors that influence behavior, including physical elements, like access to resources and services, and social elements, such as support from others and cultural influence.
- Physical opportunity: Keybarriers included:
- Cost: Participants said the price of ingredients and foods associated with the MedDi was a barrier;
- Time: Time constraints were also commonly reported, whether due to busy lifestyles or the extra time needed to plan, cook, or prepare MedDi meals;
- Physical environment: Individuals expressed challenges in their food environments, such as limited access to MedDi components, difficulty identifying them in stores, or being surrounded by less healthy food options;
- Social opportunity: Cultural influences and a lack of support from others, such as spousal disagreements about diet, also posed challenges for some.
Motivation
Motivation is the internal drive to engage in a behavior. It includes reflective motivation, such as conscious decision-making and evaluations, and automatic motivation, which involves habits and emotional responses. In the COM-B model, resistance to change is most closely associated with motivation.
- Reflective motivation (conscious thoughts and decisions):
- Several participants felt the MedDi was too different from their usual diet or didn’t fit with their cultural background;
- Others didn’t like the idea of having to follow dietary rules or restrictions;
- For some people, the gap between their current diet and the MedDi felt too big to manage.
- Automatic Motivation (subconscious processes):
- Some stated feeling helpless or unsure about how to begin making dietary changes;
- Others hesitated because they weren’t confident about fully committing to a new dietary approach;
- Struggles with willpower and staying motivated over time were also reported;
- Many participants emphasized the need to preserve their own food preferences and routines while making changes.
Translating Research into Action: How to Support Long-Term Dietary Change
Our findings shed light on a range of obstacles that make it difficult for middle-aged and older adults outside the Mediterranean region to adopt the MedDi. Some are general, such as resistance to change, while others are more specific to this diet, including cultural attachment and limited knowledge of the diet itself. A more recent review echoed many of our findings, even in a broader age range, stressing the importance of considering the specific needs of the target audience when designing dietary interventions.
By clarifying these challenges, our study provides a foundation for Luci’s approach to identifying and implementing behavior change strategies and forms of tailored support using the BCW.
- To address some of the capability-related challenges that were documented in the studies (ex: not knowing enough about the MedDi or not having strong enough cooking skills), strategies like education and building practical skills are recommended. In light of this, the Luci platform applies these strategies, for example, by providing suggestions for meal planning and tips for simple cooking to overcome a lack of food skills.
- For opportunity-related challenges, such as high cost or lack of time, strategies like enablement and training are recommended. Enablement involves providing practical support to reduce barriers or to build skills. For example, it can include tips on how to eat well on a budget.
- Lastly, motivation barriers, common in the studies we analyzed, can be tackled with strategies like offering incentives/rewards and providing practical support. In light of this, the Luci program applies these strategies by encouraging users to set specific, measurable, achievable, realistic, time-bound (SMART) goals, and self-monitor their progress by regularly tracking the evolution of these goals. This can help boost self-control and reduce feelings of helplessness, making it easier to maintain lasting behavior changes.
Fostering healthy aging through lifestyle and diet starts with understanding the real-world barriers people face and developing targeted behavior change strategies to overcome them. Addressing these key challenges is the first step toward lasting change. Programs like Luci offer promising evidence that with the right tools, structure, and support, individuals can make sustainable improvements to their eating habits and overall well-being.
Click here to learn more about the Luci program.
Authors
Roxanne Bennett is a registered dietitian from Montreal, Canada. She earned her dietetics degree from Université de Montréal in 2016 and an applied master’s from McGill University’s School of Human Nutrition in 2018, focusing on public health. Her interests range from the molecular foundations of nutrition to broader population health.
Isabelle Lussier is Director of Scientific Affairs at Lucilab. She oversees the organization’s scientific strategy and co-leads the clinical validation process of the Luci program.
Juliette Guillemont has been contributing to the Luci project since its inception. She helps ground the Luci project in science. She has extensive experience in the development and evaluation of health prevention interventions.
Guylaine Ferland is a full professor in the Department of Nutrition at Université de Montréal and a scientist at the Research Centre of the Montreal Heart Institute. Her research focuses on the nutritional determinants of cognitive health during aging. Her work on vitamin K and cognition is recognized internationally. She is a fellow of the Canadian Nutrition Society.
Sylvie Belleville is a full professor in the Department of Psychology at the University of Montreal and a researcher at the Research Centre of the Montreal Geriatric University Institute. Holder of the Canada Research Chair in Cognitive Neuroscience of Aging and Brain Plasticity, she is recognized for her work on cognitive changes related to aging and mild cognitive impairment, on programs to reduce their impact, and on their implementation in the community.
