HPV Vaccination is Not Just for Kids: Communicating Effectively to Promote Cancer Prevention on College Campuses
Today, March 4, 2019 is the second annual International HPV Awareness Day, which aims to promote education and awareness about the human papillomavirus (HPV). And, with recent news that the vaccine is now FDA-approved in the US for adults 27-45, communication strategies about the vaccine and its scientific efficacy are changing. In the following piece, Dr. Katharine Head and MD/MPH student Katheryn Schloss discuss their innovative approach to encouraging college students to increase awareness and get vaccinated. –KHL
By Katharine J. Head, PhD, Indiana University School of Liberal Arts & Katheryn N. H. Schloss, MD/MPH Student, Indiana University School of Medicine
According to the US Centers for Disease Control (CDC), HPV is the most common sexually transmitted infection in the world – so common that an estimated 80% of all sexually active people will get the virus at some point in their lives. While most infections clear on their own, persistent infections with some strains of HPV can lead to cancer. These HPV-attributable cancers are responsible for more than 42,000 new cases of cancer each year in the US, and include almost 100% of cervical cancers, as well as vaginal, vulvar, penile, anal, rectum, and most oropharyngeal cancers. Some types of HPV are also known to cause genital warts.
There is no treatment for HPV, and, for many years, cancer screenings were the main tool for combating HPV-attributable cancers. But, all that changed about 13 years ago, with the incredible development and dissemination of the multi-dose HPV vaccine, one of the first primary cancer prevention innovations in the world. The early vaccine prevented four types of HPV (6, 11, 16, and 18). This quadrivalent vaccine was designed for use in females aged 9 to 26 years in the US in 2006. Three years later, in 2009, it was further licensed for use in males. Then, in 2015, a nine-valent vaccine (HPV Types 6, 11, 16, and 18, plus five additional types, 31, 33, 45, 52, and 58) was introduced into clinical practice. This version of the vaccine has been shown to be very safe and very effective, providing high levels (over 90%) of protection against these oncogenic (cancer-causing) HPV strains, as well as the strains that cause genital warts.
HPV Vaccine Rates Still Low in the US
Unfortunately, despite its availability for over a decade, HPV vaccination rates remain low in the US. Per 2017 CDC data, only 48.6% of all 13-17 year old males and females in the US have completed the HPV vaccination series. When separated by sex, 53.1% of 13-17 year old females and 44.3% of 13-17 year old males have completed the HPV vaccination series. Our rates are well below the Healthy People 2020 goal of 80% vaccination rates, which was deemed consistent with achieving good herd immunity for our society. As these data suggest, many emerging adults are not protected against HPV.
Messaging About Vaccines to Varied Audiences
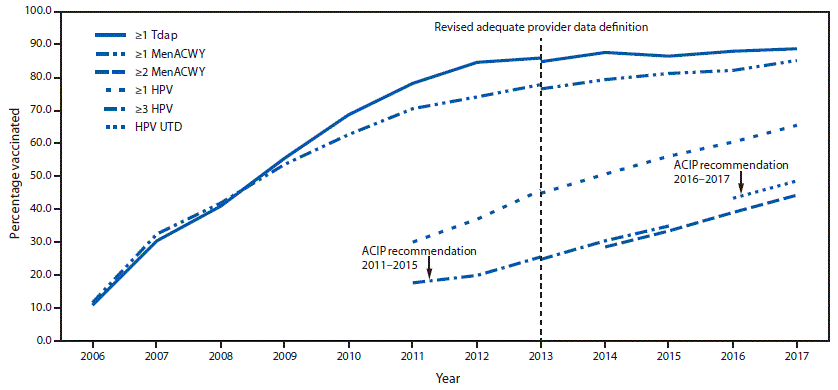
The majority of work promoting the HPV vaccine has been directed at parents of children who are 11-12 (the optimal age for HPV vaccination, according to the CDC). While other age-appropriate vaccinations are high for this age group (see Figure 1), many parents choose not to get the HPV vaccine, representing a “missed opportunity” for many adolescents. Communication about HPV vaccination has also been tinged with discussions of sexual behavior and perceptions that the vaccine was rushed into approval. This has made promotion of the vaccine to parents of adolescents somewhat difficult. However, research has shown that the most effective strategy is a strong provider recommendation given in the context of other childhood vaccines at 11-12 years old.
On the other hand, there has been limited work promoting and addressing the vaccination behaviors of young adults. Currently, the HPV vaccination is recommended up to age 26. But, with the recent licensing of the vaccine up to age 45 for both males and females, there will be a growing need to understand how we promote this vaccine to unvaccinated adults.
The messaging around HPV vaccination is different for young adults than it is for parents of adolescents. Research shows, for example, that young adults are interested in issues of susceptibility and transmission when thinking about getting the HPV vaccine. College and university campuses are an ideal place to promote this vaccine to young adults: most students are over age 18 and able to consent, many colleges and universities have an on-campus health center or clinic where vaccines can be administered, and the campus itself provides an insulated environment in which promotion and education about the vaccine can be easily accomplished.
A Campaign at IUPUI
We recently undertook two different initiatives to promote HPV vaccination on our college campus: Indiana University Purdue University Indianapolis (IUPUI). Indiana has below national average HPV vaccination rates – ranking 40th in the country for both 1st dose and 3-dose series completion. Of particular concern is the low vaccine uptake for males, with Indiana ranking 43rd in the country. Not surprisingly, we also have above average rates of HPV-attributable cancers. While many efforts to increase uptake in Indiana have focused on younger ages, we recognized a need to increase HPV vaccination in those in the older approved age range, particularly males. Given that over 85% of IUPUI students are from the state of Indiana, we knew that many of our own students were unvaccinated – and representative of our state’s poor HPV vaccination rates.

So what did we do?
- A six month (April to October of 2018) campaign which included: a) theory-informed, campus-wide education and promotion about HPV and the vaccine which cued students to visit campus health clinics (see sample posters, placed in bathroom stalls and in digital signage around campus), b) training campus health professionals to answer questions and give a strong HPV vaccination recommendation, c) a text message reminder system for subsequent vaccine doses. Our campus went through the process of becoming a Vaccine for Children and Indiana State Department of Health Adult Immunization Program member, which ensured that students without insurance coverage would be able to get vaccinated for no cost. This effort resulted in a total of 485 HPV vaccine doses given during the six-month period, which represents a 635% increase compared to the same six-month time period in 2017. Of particular note is that the percentage of males who were getting vaccinated increased from 17% to 38%.
- A one-day mass vaccination clinic in October 2018, which not only offered HPV vaccination, but also influenza and meningitis B (a requirement for all incoming students starting in Fall 2018 at our university). Social media posts, emails to students, and articles in the campus newsletter promoted the event and highlighted that vaccines were being given at no cost.. Day-of promotion consisted of signs advertising the event, along with vaccination-themed giveaways (t-shirts, lanyards, stickers, etc.) for students who came through the clinic. We gave 784 influenza vaccine doses, 500 meningitis B vaccine doses, and 378 HPV vaccine doses to 901 students during this single-day event.

These efforts reveal that college campuses can be a prime setting to communicate effectively about the HPV vaccination, whether through a long-term campaign or a one-day event. It’s important to note that both projects were a collaboration between our team, campus health, campus administration, state department of health, regional non-profit organizations, and student leaders from various organizations on campus. Integral to the success of both efforts, as is the case for most work in public health, was the collaborative approach we took in designing and implementing our interventions.
We are hopeful that in the coming years, many more adolescents will be vaccinated at the recommended age of 11-12 years. Like any vaccination, high herd immunity is needed for us to reap the full benefits of HPV vaccination. In fact, the World Health Organization has recently declared that the elimination of cervical cancer is “within reach” due in large part to the HPV vaccine.
Given current low vaccination rates for adolescents, coupled with a lack of work targeting young adults, we hope to raise awareness about the potential for colleges and universities to play an integral role in promoting the HPV vaccination to their students. The messaging and promotion of HPV vaccination for young adults will need to be different than it is for adolescents, and researchers and practitioners alike must step up and embrace this challenge.
So, we encourage you to celebrate today, International HPV Awareness Day, by learning more about the HPV vaccination and encouraging college students or any young people you know to get vaccinated. Who knows? You could just save a life.
Want to stay connected with #SciCommPLOS or pitch an idea for a blog post? Tweet us at @SciCommPLOS or email us at scicommplos@gmail.com.
